Here’s a quick case study of a slightly unusual case (told with the patient’s permission) that came through work a couple of weeks ago. In a similar fashion to my mate who was shot through the neck by an AK 47 round whilst fighting Taliban in Afghanistan (for that full story click here), the current casualty was engaged in the equally manly pursuit of pig hunting with nothing but a dog and a spear! Located in a remote area of Central Queensland, and with a large wild boar bailed up by his pig dog, in the heat of the moment whilst hurdling a fence to get to the pig, the casualty slipped and fell, impaling himself on his own spear in the process.

From a medical perspective it is never recommended practice to remove any penetrating foreign body until in the appropriate medical facility, the concern being that the penetrating foreign body may have hit a major blood vessel, but be tamponading, or preventing the vessel from bleeding. Once removed, the vessel may be free to bleed, and hard to control in the pre-hospital setting. The casualty found himself with the dilemma of being a four-hour walk and a short boat ride from the nearest hospital, and faced with no other option than to remove the spear to start his exfiltration. Further complicating the situation was that the casualty and his hunting partner had not packed their full medical kit for the hunt, having only a rudimentary kit with some simple bandages at hand (for a guide to a good medical kit for hunting see the article linked here). On removing the spear, the casualty fortunately found that the bleeding from the wound was minimal, and was easily controlled with a compression bandage. He then started the arduous journey back to hospital where I met him some four hours later.
On initial review, and as with any limb injury penetrating or not, my highest concern was for the nerve and blood supply to the leg and foot beneath the wound. The history from the casualty that the bleeding was relatively easy to control was somewhat reassuring that he hadn’t severed any major blood vessels, but the location of the wound was highly concerning for a posterior tibial artery injury.
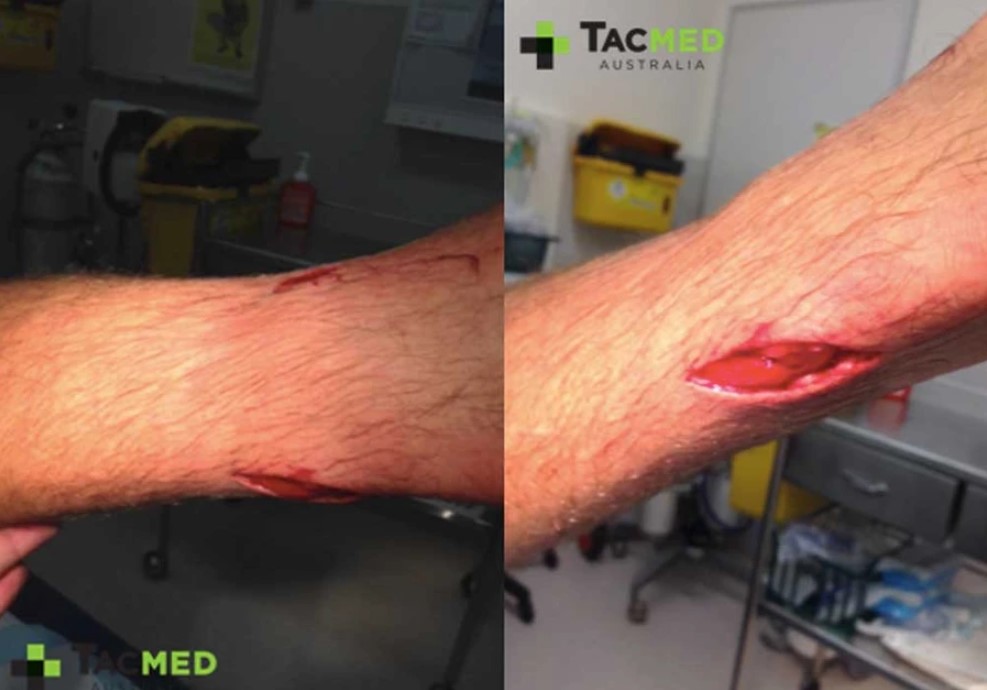
Thankfully the casualty had a strong posterior tibial pulse distal to the wound, with good blood supply and full sensation and movement in the foot suggesting no significant nerve damage. Once I had ascertained that the foot was neurovascularly intact, the next step was to assess the wound itself. With an appropriate supply of new compression bandages at hand in case the wound bled once the dressing was removed, I took down the dressing and revealed the wound pictured above. It was immediately apparent that due to the severity of the wound, as well as the contaminated nature of the spear tip, that this wound required a surgeon to explore and thoroughly clean it out. Given that the casualty was over four hours post-injury my other primary concerns were tetanus prophylaxis and intravenous antibiotics. An X-ray was organised which showed no bone damage and no obvious retained foreign bodies in the wound. The soft tissue image provided by the X-ray suggests that the spear had passed relatively superficially through the tissues of the inner lower leg, as seen on X-ray by the slightly darker soft tissue shadows where air has entered the wound.
After some pain relief, a tetanus booster, a loading dose of intravenous antibiotics, and an initial wound washout to reduce the bacterial load in the wound, the casualty was sent off to the surgeons for an uncomplicated exploration and washout under anaesthesia followed by wound closure.
All in all it was a good outcome for the casualty, however the situation could have been much worse if he had have cut his posterior tibial artery, or if the spear had have penetrated another region of his body, for example his abdomen or chest. The take home points for the casualty were to always have an appropriate medical kit at hand to deal with likely injuries that might occur whilst hunting, including significant bleeds, as well as a comprehensive medical evacuation plan if it all goes wrong. In his setting an EPIRB might have been a very handy bit of equipment to have at hand if the injury had have been more significant and he wasn’t able to walk out.
From a medical perspective the key points were to rapidly assess neurovascular function below the wound, being prepared for a significant bleed when the dressings were taken down, and to recognise early that this was a wound that a surgeon needed to look at. Furthermore, a good history of the mechanism of injury allowed the early recognition that tetanus prophylaxis and intravenous antibiotics were a priority, as well as an initial wound washout to decrease the contamination in the wound prior to a proper surgical washout.
Thanks for reading, as always comments and questions are welcome. Cheers, dan.